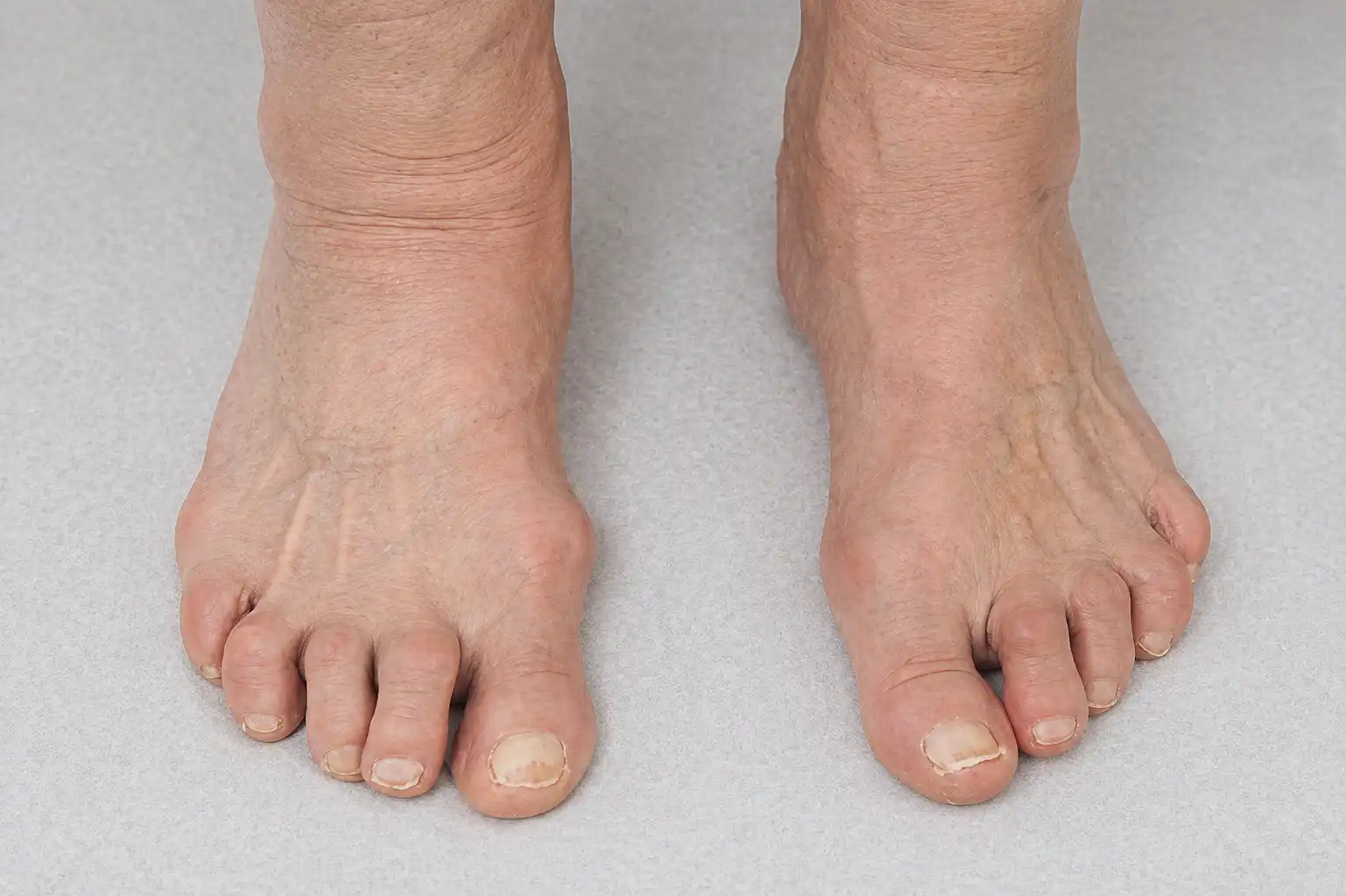
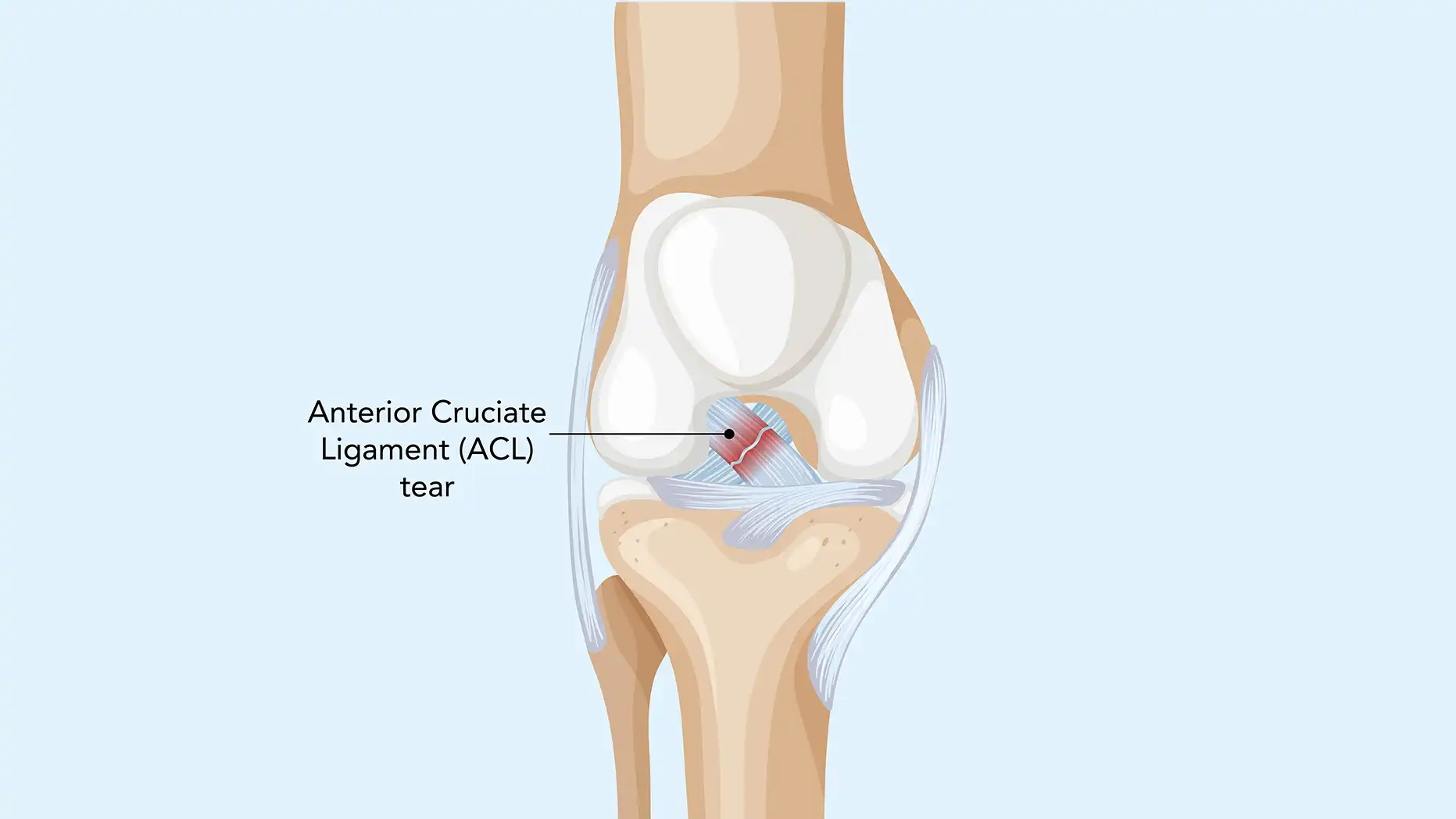
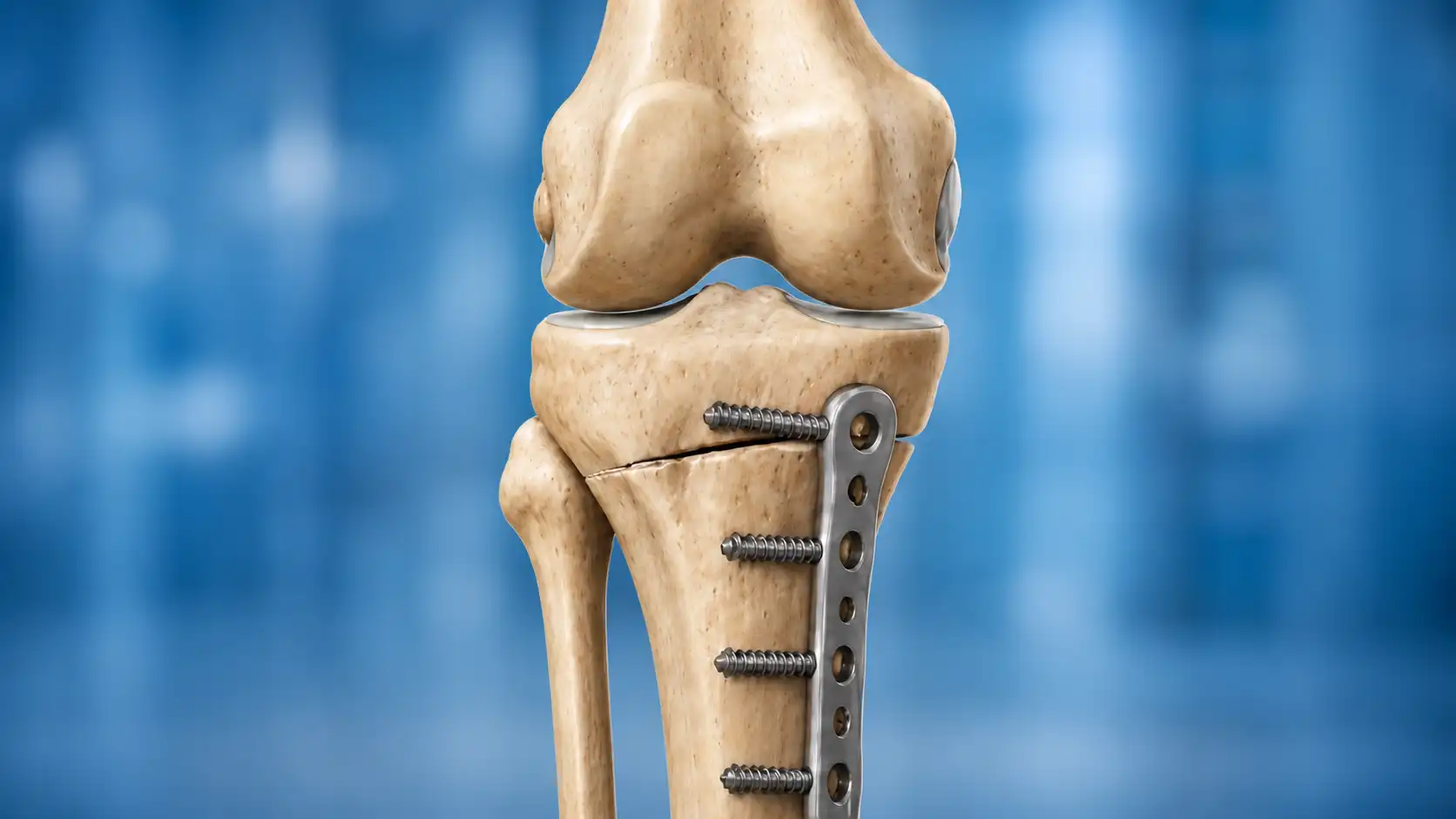
Why Foot Arthritis Often Goes Unnoticed
Foot pain rarely starts as something severe. It often begins with mild discomfort after walking or stiffness in the morning. Many people carry on and assume it will pass.
Over time, arthritis in feet develops quietly. The joints begin to wear down, movement becomes limited, and pain becomes more frequent. What feels minor at first can slowly affect how you walk, stand, and move each day.
What is Arthritis in Feet? A Simple Explanation
Rheumatoid arthritis in feet is an autoimmune condition where the immune system attacks the joint lining, causing inflammation, pain, and potential structural damage. Management often requires specialist rheumatology input alongside orthopaedic care.
This condition can affect the toes, midfoot, and ankle, leading to reduced flexibility and ongoing discomfort.
Why Does Arthritis Develop in the Feet?
The feet support your full body weight every day. Over time, this constant load places stress on the joints, especially if there are underlying risk factors.
Common Causes of Arthritis in Feet
- Age-related cartilage wear
- Previous foot or ankle injuries
- Autoimmune conditions like rheumatoid arthritis in foot and ankle
- Structural issues such as flat feet or high arches
- Repetitive strain from prolonged standing or walking
These factors gradually increase pressure on the joints and lead to inflammation.
The Three Types of Arthritis That Affect the Feet Most Often
The Three Types of Arthritis That Affect the Feet Most Often
Osteoarthritis in feet
The most common type. This is classic wear-and-tear arthritis, where cartilage slowly erodes over years. It tends to develop gradually in people over 50, though younger patients with a history of injury or physically demanding activity can be affected too.
Rheumatoid arthritis on feet
An autoimmune condition in which the body’s immune system attacks the joint lining. It often affects both feet simultaneously, typically starting in the smaller joints of the toes. Around 90% of people with rheumatoid arthritis will develop foot and ankle symptoms at some point during the course of the condition.
Post-traumatic arthritis
This develops after an injury to the foot or ankle, a fracture, severe sprain, or dislocation, even one from many years ago. The initial joint damage accelerates cartilage deterioration over time, often catching patients off guard.
Identifying the correct type is the first step we take before recommending any course of action. It directly shapes how we treat you.

Could Your Old Sports Injury Be the Real Cause of Your Foot Pain Today
This is something that surprises many of our patients. An ankle sprain from years ago on the football pitch, a stress fracture from running, or a dislocation that seemed to heal completely at the time, all of these can cause cartilage damage that is not immediately obvious.
Over the following years, that hidden damage accelerates joint wear, eventually leading to post-traumatic arthritis. If you have a history of foot or ankle injuries and are now experiencing joint pain, stiffness, or swelling, the two are very likely connected.
For a broader understanding of how previous injuries can affect joint health, you can explore our knee sports injuries and trauma page, where we explain how injury-related joint damage develops over time.
Early Signs People Often Ignore
Symptoms often develop slowly. Many people do not realise they are dealing with joint changes until movement becomes difficult.
Symptoms of Arthritis in Feet
- Feet stiff in the morning
- Pain during or after walking
- Swelling around joints
- Reduced range of motion
- Feet pain while walking
- Painful legs and ankles
Morning stiffness lasting more than 30 minutes may suggest an inflammatory arthritis rather than osteoarthritis and warrants early specialist assessment.
These early signs are important and should not be ignored if they continue.
Arthritis in Big Toe: A Common but Overlooked Problem
The big toe plays a key role in balance and walking. When this joint is affected, even simple movement can feel restricted.
What is Hallux Rigidus?
Hallux rigidus is a type of arthritis that affects the big toe joint. It causes stiffness and pain, especially when pushing off during walking. It is one of the most common forms of arthritis in big toe.
Signs of Arthritis in Big Toe
- Pain when walking or standing
- Stiffness in the toe joint
- Swelling around the joint
- Difficulty bending the toe
Recognising arthritis in big toe symptoms early can help prevent further joint damage.
Arthritis in Feet and Ankle: Understanding the Connection
Why the Foot and Ankle Are Affected Together?
The foot and ankle work as a connected system. Every step you take involves multiple joints moving together to absorb load, maintain balance, and propel you forward. When arthritis develops in one part of this system, it often places increased stress on the joints around it.Osteoarthritis commonly affects the ankle joint, the midfoot, and the hindfoot, the group of small joints at the back of the foot that controls side-to-side movement. When these joints become stiff or painful, the ankle often compensates, which over time can lead to further wear and inflammation.
Symptoms That Suggest Ankle Involvement
If your foot pain extends beyond the toes or midfoot, ankle arthritis may also be a factor. Signs to look out for include:
- Pain or stiffness around the ankle after rest or activity
- Swelling on the inner or outer side of the ankle
- A feeling of instability or giving way when walking on uneven ground
- Reduced ability to move the ankle up or down
These symptoms can develop alongside foot arthritis or independently, and it is not uncommon for patients to present with both.
Why Early Assessment Matters
Arthritis in the foot and ankle is often underdiagnosed because the symptoms can feel similar to a sprain or general overuse. A proper clinical assessment, supported by imaging, helps identify exactly which joints are affected and to what degree.
Understanding whether the ankle is involved changes the treatment approach. Targeted injection therapy, footwear modification, and physiotherapy can all be adapted to address both the foot and ankle together, rather than treating each in isolation.
If you have persistent pain across the foot and ankle, an early assessment gives you the best chance of managing the condition before it progresses further.
When is Foot Arthritis a Concern?
It is common to feel occasional foot discomfort. However, persistent or worsening symptoms may indicate something more serious.
Mild vs Serious Symptoms
| Mild symptoms | More serious signs |
|---|---|
| Occasional stiffness | Constant or worsening pain |
| Pain after longer periods of activity | Swelling that does not settle |
| Reduced ability to move the foot | |
| Difficulty walking even short distances |
If you are unsure whether your symptoms are progressing, we can assess this quickly and help you understand what is happening.
How is Arthritis in Feet Diagnosed?
Understanding the exact cause of your symptoms is essential before starting treatment. Many conditions can feel similar, which is why a proper assessment matters.
What to Expect During Assessment
We begin with a detailed discussion about your symptoms and how they affect your daily life. We then examine movement, swelling, and joint function.
You may also need imaging such as X-rays to confirm the diagnosis and assess severity. We focus on giving you a clear explanation so you understand what this means and what to do next.
Grading the Severity of Arthritis
Arthritis is typically graded from mild to severe based on imaging findings. Understanding the stage of your arthritis allows us to match the right treatment, from conservative management in early stages to surgical options in advanced cases. Your X-ray or MRI results will inform this discussion at your consultation.
Treatment Options for Arthritis in Feet
Treatment depends on how advanced the condition is and how much it affects your mobility. The aim is to reduce pain and support movement.
Non-Surgical Treatment Options
- Physiotherapy to improve strength and flexibility
- Supportive footwear or orthotics
- Anti-inflammatory medication
- Injection therapy, including advanced options such as Arthrosamid®, a hydrogel injection that cushions the joint and reduces pain suitable for patients looking to delay or avoid surgery.
These options form the foundation of arthritis in feet treatment and can help manage symptoms effectively.
When Surgery May Be Considered
If symptoms continue despite treatment, surgery may be considered. This is usually for more advanced cases where joint damage is significant. For hallux rigidus, surgical options may include joint preservation procedures or fusion, depending on the stage of damage and your activity level. Mr Khakha will discuss all options based on your imaging and symptoms.
Arthritis in Big Toe Treatment Options
Big toe arthritis can significantly affect walking, but early management can make a difference.
Managing Hallux Rigidus
- Footwear changes to reduce pressure
- Exercises to maintain joint mobility
- Injections to control inflammation
In some cases, surgical options may be discussed if movement becomes very limited.
What to Expect From Recovery and Long-Term Management
Arthritis is a long-term condition, but it can be managed with the right approach. Many patients ask if it will improve. While will osteoarthritis get better is a common question, the focus is on controlling symptoms and maintaining function.
With the right care, many people continue their daily activities with improved comfort and mobility.
When Should You Seek Medical Advice?
You should consider seeking medical advice if symptoms begin to affect your daily life or do not improve over time.
- Pain lasting more than a few weeks
- Persistent swelling
- Difficulty walking or standing
- Increasing stiffness
If you are experiencing these symptoms, we can help you understand the cause and guide you on the next steps.
What to Expect at Your First Appointment
Your appointment begins with a detailed conversation about your symptoms, when the pain started, what makes it worse, and how it is affecting your daily life. Our doctors will then examine your foot and ankle, assessing movement, swelling, and joint function directly.
Where needed, X-rays are arranged to confirm the diagnosis and assess the degree of joint damage. In some cases, an MRI scan may be recommended to provide a more detailed picture of the soft tissues and cartilage.
By the end of your appointment, you will have a clear understanding of what is causing your pain, how advanced the condition is, and what your treatment options are. There is no pressure to make immediate decisions. The aim is to give you the information you need to move forward with confidence.
You do not need a GP referral to book.

How We Help You Move Better at London Knee Care
At London Knee Care Clinic, we focus on helping you understand your symptoms clearly and act early.
We know that ongoing foot pain can be frustrating and uncertain. Our role is to give you a clear diagnosis and a practical plan that fits your daily life.
When you come to us, we assess your condition in detail and explain what is causing your pain. We guide you through the most suitable treatment options, whether that involves physiotherapy, injections administered under image guidance for precision and safety or further intervention.
All assessments and treatments are led by Mr Raghbir Khakha, a consultant orthopaedic surgeon with specialist expertise in joint preservation and knee conditions. He works from leading London hospitals, ensuring you receive consultant-led care from your first appointment.
If you are unsure about your symptoms, you can book an appointment with us and we will assess this quickly. We aim to give you clarity and reassurance from the first visit.
You can take the next step by visiting our contact us page or book your appointment online at a time that suits you.
We make the process simple, so you can focus on getting back to comfortable movement.
Frequently asked questions about arthritis in feet
Can rheumatoid arthritis cause swollen feet?
Yes, swollen feet and rheumatoid arthritis are often linked. This condition causes inflammation in the joints, which can lead to visible swelling, warmth, and discomfort.
If swelling is persistent or painful, we can assess the cause and guide you on the next steps.
What causes feet and ankles to swell?
There are several reasons what cause feet and ankles to swell, including fluid retention, injury, or joint inflammatio
When swelling is ongoing and combined with stiffness or pain, arthritis may be a contributing factor. A proper assessment helps identify the exact cause.
What are the symptoms of arthritis in big toe?
Common arthritis in big toe symptoms include:
- Pain when walking or pushing off
- Stiffness in the joint
- Swelling around the toe
- Reduced movement
These symptoms often develop gradually and can affect daily mobility.
How is arthritis in big toe treated?
Arthritis in big toe treatment depends on severity. Early stages are usually managed with non-surgical care.
How to treat arthritis in big toe?
- Footwear changes to reduce pressure
- Physiotherapy to improve movement
- Anti-inflammatory treatment
- Injections for pain relief
If symptoms progress, we guide you through further options based on your condition.
What causes arthritis in feet?
Common answers to what causes arthritis in feet include joint wear over time, previous injuries, and conditions like rheumatoid arthritis. Foot structure and daily stress on joints also play a role. Identifying the cause helps determine the right treatment plan.
Is it arthritis in big toe or gout?
Many people wonder if it is arthritis in big toe or gout. Both conditions affect the same joint but behave differently. Gout usually causes sudden, severe pain with redness. Arthritis develops slowly with stiffness and reduced movement.
Gout can be confirmed through blood tests measuring uric acid levels, whereas osteoarthritis is typically diagnosed through clinical examination and X-ray. We can help you distinguish between the two with a proper assessment.
Will osteoarthritis get better over time?
A common question is will osteoarthritis get better. Osteoarthritis does not reverse, but symptoms can be managed effectively. Research and NICE guidelines confirm that targeted physiotherapy, weight management, and appropriate injection therapy can significantly reduce pain and improve function in the majority of patients. With the right treatment, many people experience improved movement and reduced discomfort.